How to treat postpartum depression naturally
Read about Dr. Erika’s personal story about postpartum depression here. I’m going to talk today a little bit about how to treat postpartum depression naturally, and some things you may want to speak to your doctor about if you think you have postpartum depression or anxiety.
The very first thing we should talk about is some lab work. So when we talk about treating postpartum depression naturally I really want to know why someone has postpartum depression, and not to just treat it presumptively. (In other words – is it really postpartum depression?) So the first thing I want you to talk to your doctor about is getting some basic bloodwork done.
The first thing I like to order is a Complete Blood Count (or “CBC”) to see the size and shape of your red blood cells and white blood cells. If you have too low of red blood cells (anemia) that can be a frequent cause of fatigue and depression. An add-on test to that would be something called a serum ferritin, which checks the storage form of iron. This is a much more reliable test than a serum iron because serum iron levels can fluctuate, whereas the ferritin stays relatively the same. If you did have anemia or iron deficiency in pregnancy then this test is even more important (though I think everyone should get checked in postpartum, just in case).
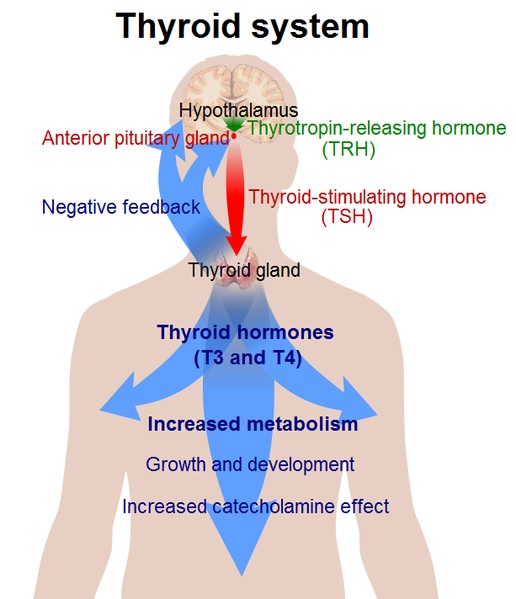
The next thing you should do is have your physician check you for postpartum thyroiditis. Postpartum thyroiditis occurs in over 5% of women (that’s a lot of women), and remember that the symptoms can mimic depression very closely. Check out the full blog post about postpartum thyroiditis and postpartum depression. You should also check your vitamin D if you hadn’t at some point in pregnancy. The best test for this is 25-OH (hydroxy) vitamin D. Your checklist for labwork:
- A CBC (with differential, to be precise)
- A serum ferritin
- Thyroid panel (see the full video about thyroiditis to see what I recommend)
- 25-OH vitamin D.
Your physician may choose to do a few more tests, too (like a metabolic panel or urinalysis). The next thing I do for women with postpartum depression is to check their gut. I’m not totally sure why this is, but I seem to see a lot crossover between gastrointestinal symptoms/abdominal pain and depression and anxiety, which I think is pretty interesting. So you if have any symptoms like gas, bloating, diarrhea, constipation (or alternating diarrhea and constipation), fatigue or brain fog – these may be symptoms of gut dysbiosis. Dysbiosis is simply the overgrowth of abnormal bacteria.
Pretty interesting – very recently there was a study that came out that reserachers could induce anxiety in mice just by changing their gut flora. They took the gut flora from anxious mice and put it into normal mice and made them anxious (and vice versa, they took good gut bacteria and fed it to anxious mice and saw that their anxiety decreased). I think that’s pretty cool. It is something that naturopaths have been saying for years (decades now!) about the relationship between gut health and mood.
There’s a lot to say about treating the gut. One is definitely removing food allergens. That is something we need to be a little careful about in the postpartum period because consuming calories – making sure you have enough calories to maintain lactation to be able to nurse your baby – takes priority over us really healing your gut at this point. But that said, if you have known food “allergens” (sensitivities) like a gluten sensitivity or a dairy sensitivity this is a good time to check in on those foods and eliminate them whenever you can, as long as you can maintain enough calories to sustain nursing. (Side note: a true food “allergy” is the anaphylactic kind, most people have food sensitivities. I misspeak a little in the video, and I want to keep my terminology straight!)
The next thing I like to do for folks who do have gastrointestinal complaints is give them very high quality probiotic. All high quality probiotics should be somewhere in the thirty and forty dollar range. If you’re buying a ten dollar probiotic chances are those an organisms aren’t alive anymore and and that’s not such a good thing. I really like the Klaire Labs brand probiotic (I don’t get any money from endorsing them, though it would be nice if I did!) – they are a little harder to find. I also like the Culturelle brand probiotic, which you can find most places.
Another thing that I like to do for folks – this can be related to the gut, but is more related to brain chemistry itself – is to get on a good high quality fish oil as well. I really like the Pharmax brand – Nordic Naturals and Carlson’s are also pretty good. (Still don’t get paid to endorse them, though the Nordic Naturals link is through my Amazon account, if you’d like to support this blog.) I prescribe at least 5 grams per day of combined EPA and DHA. Normally we think about DHA being great for brain development – which it is – that’s what we give our moms in the prenatal period to make sure the baby’s brain development is good. It’s important to supplement DHA, but it is actually the EPA component that seems the best for anxiety and depression. So I want you to get one that has both. Make sure you speak with you physician about that – there are a few women that this is not an appropriate prescription for.
The next thing I’d like to talk about is getting folks on a really good quality multivitamin. I use the Thorne brand here in my office (still no affiliation). I know I’m talking about brands a lot, and that is because it seems that brand do matter when it comes to efficacy. At the least, I have found that switching folks from a low (Costco) or even medium quality (Good Food Store) brand to Thorne/Pharmax, etc, it makes a big difference. (Read more here about why picking a high quality multivitamin is so important.) Make sure to keep taking your prenatal vitamin all the way through postpartum – for as long as you are nursing your child (and possibly longer). Remember that if you’re nursing your little one is sucking all those nutrients out of you via your breast milk. That’s why taking a good quality prenatal vitamin and fish oil is so important – if you are losing important fats and nutrients it can contribute to fatigue and depression.
Sometimes women just don’t have enough B vitamins to get through the day. Speaking of B vitamins – that’s the next thing I like to do for folks. If the regular prenatal vitamin isn’t quite enough, or if you are feeling really fatigued or stressed out, you can start on a basic B vitamin. This one is a bit trickier to say who should do what and how much to take. It’s a bit more personalized – B vitamins definitely aren’t for everyone, and there’s some safety data that’s lacking for certain B vitamins and certain doses in the postpartum period in lactation. Check with your physician about that one as well.
I should also mention that exercise is probably the best thing that you can do for yourself in the postpartum period to prevent depression or to treat depression. There is tons and tons research on how important and really effective exercise is in improving depression. There are even research studies that compare exercise to SSRI’s and anti-depressants. Exercise inevitably wins! That is really neat. I know that can be really difficult for a lot of women in the postpartum period to exercise. You’re tired, you’re stressed out, you’re really really busy – but it’s really important to make sure you get outside in at least take your little one for a walk every day at least 30 minutes. You will notice your mood improves pretty significantly.
Make sure you get exposure to good bright light during the day if you can. If you live in the Pacific Northwest’s or Alaska or some of those gray areas of the country, I do recommend getting one of those broad spectrum lightboxes (like a Happy Lite) those can be really helpful for for seasonal affective disorder (SAD) patients that are really sensitive to light. Finally, the very last thing that you can speak with your physician about if all of these other things haven’t been quite enough… And I know these things seem really basic – but I’ll be honest, in about half or more than half of cases in my practice, just the things I have mentioned so far have really turned a lot of women around.
The last thing you can consider speaking with your physician about is getting a prescription for progesterone. In pregnancy progesterone levels are really really high. Progesterone actually acts on the GABA receptor in the brain – which means that it acts like Valium in the brain. So you can imagine why you normally feel pretty happy in pregnancy (well, maybe not so great otherwise, but usually mood is pretty good). In the postpartum period there is a very sudden drop in progesterone and for a lot of women that can really trigger some severe depression and anxiety. Because – that vallium is taken away! So what we can do for some women who are experiencing very severe depression or anxiety is to replace progesterone for a time so that we can more closely control the weaning off of progesterone. That would be 100 to 200 milligrams of oral micronized progesterone, also known as Prometrium. It is a peanut oil product, which is very frustrating, so if you are allergic or sensitive to peanuts it may not be appropriate for you. Once again, it can be very helpful for some women, but you have to talk to your doctor about that one – it is not perfect for everyone.
I’ve got lots more tricks up my sleeve for postpartum depression anxiety treatment. Usually it involves a lot of evaluation of women. I am looking out for further food allergies and sensitivities, I check nutrient balance and look at diet, make sure folks are getting enough protein, and lots of other lifestyle factors. I will speak a little bit more about those in future episodes. I hope you enjoyed this! Please comment under this blog post if you have any other questions or need clarification.
In HOPE and good health, Dr. Erika


Carrie
January 3, 2014 at 11:07 pmReally great post. Thank you.
Maheen Ahmed
December 19, 2013 at 11:33 pmI love the information being provided in this article. You need the most effective techniques and approach to help the human body heal itself naturally and that can be achieved by simply pushing the mind in moving out
of the way and activating the parasympathetic nervous system. Learn more about it http://www.howtoOvercomeAnxiety.org