
Failure to Thrive in a Breastfed Baby
If your baby has failure to thrive please read the first part of this blog post at: What to do if your child drops on their growth curve or is diagnosed with Failure to Thrive
Contact an IBCLC first
If your baby is breastfed and is not gaining appropriately I highly recommend working with a lactation consultant (IBCLC). Click here to find a lactation consultant near you
I also highly recommend checking out kellymom.com which is the internet’s best source for reliable breastfeeding information. Here are some great articles:
When to (not) supplement
First – do not start supplementing with formula, solids, or even donated breastmilk until you have exhausted all other options. This is not because supplementing is necessarily “bad.” (MOMS – please do not feel guilty if you need to supplement, you are still a good Mom!) BUT – it can be very difficult to regain milk supply when the baby is getting supplemental milk. Please wait until your physician advises you to supplement or when you have tried everything else first.
Generally speaking, babies who have lost more than 7% of their body weight and have not regained it by 7 days will probably need to supplement. Additionally, babies who do not have enough wet or poopy diapers may need to supplement, as this may indicate dehydration or lack of nourishment. Remember that babies should have 1 wet diaper on their first day of life, 2 on their second day, 3 on their third day, etc, until they reach 6+ wet diapers per day. Babies should also pass meconium (the thick, black, sticky tarry poops) within their first few days of life, and should have 3+ normal “Breastmilk” stools by day 4. (Breastmilk poops are yellowish and “seedy.”) After the first few weeks it can be normal for breastfed babies to have anywhere from 3+ poops per day to only 1 poop every 1-2 weeks. Speak with your doctor immediately if your baby is not having enough wet or poopy diapers.
Find the underlying cause: baby first
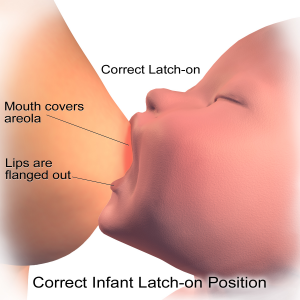
Remember that there are multiple factors that could contribute to poor growth in an exclusively breastfed baby. Rule out problems with the baby first – poor latch, tongue tie or lip tie, reflux/GERD, inattentive/stressed behavior. Many, many problems with “insufficient lactation” are due to a baby with a poor latch or sucking reflex.
Here is a great article about how to know if your baby has a good latch. And here is an awesome video showing a baby (finally!) getting a good latch.
Work with your lactation consultant to determine how much breastmilk your baby is actually getting. Your baby should be weighed before and after a nursing session to approximate the number of ounces she received. Most babies take in an average of 19-30 ounces of breastmilk per day between the ages of 1 and 6 months. Check out this breastmilk calculator
Find the underlying cause: Mom next
If your baby is having no problems, it may be your milk supply. Focus on the basics first: rest, relaxation, hydration, nutrition. Many naturopathic physicians prescribe the “24 hour” or “48 hour” cure. This involves keeping Mom and Babe together (rooming in or cosleeping safely) for a full 1-2 days. Mom is not allowed to cook, clean, do laundry, or do anything other than relax in bed with close snuggles to the little one. Family members or friends bring high calorie, nutritious food and drinks to Mom bedside so she can relax. This really WORKS!
If Mom is still struggling to produce then natural herbs or medications can be given to increase milk supply. See our post Herbs to increase milk supply: a guide to galactagogues (milk producing herbs). Absolutely make sure you continue to take your prenatal vitamin throughout the duration of breastfeeding. Some Moms may need additional iron and zinc to help the child “catch up” with growth.
Make sure you work with your physician (OB/midwife, naturopathic physician, or family practice physician) to rule out medical causes of low breastmilk supply. You should be screened for anemia (Complete Blood Count), iron deficiency (ferritin, and sometimes TIBC), thyroid disorders (TSH, and if necessary free T3 and free T4, anti-TPO antibodies, and anti-TG antibodies), and diabetes or insulin-related conditions (fasting blood sugar or complete metabolic panel will usually be ordered). Retained placenta, postpartum hemorrhage or PCOS could also affect breastmilk supply.
Don’t forget that there are many medications that can interfere with breastfeeding too. (Birth control pills are probably the most common thing to reduce milk supply.) Occasionally other things like progesterone cream or pills (sometimes prescribed for postpartum depression), or high dose vitamin B6 can also reduce breastmilk supply.
Tips to increase milk quantity and quality
Remember to feed “on demand” every 2-4 hours as needed. Do not withhold nursing sessions from a baby who has failure to thrive. Encourage the baby to completely drain the breast to get plenty of fat-rich hindmilk. Sleep near your baby (room-in or cosleep safely) or wear your baby to encourage the release of prolactin. You can also try “Kangaroo care” which is direct skin-to-skin contact with your baby – take off your shirt and the baby’s clothes (except his diaper) for at least 15 minutes or as long as you can. This encourages prolactin production and decreases stress hormones for both Mom and babe. (Stress can interfere with both milk production and “let-down.”)
You can also try pumping for 5-10 minutes after the baby finishes nursing to stimulate additional milk supply and to pump the fat-rich hindmilk. Try giving the hindmilk to the baby as a supplement (if she takes a bottle).
If your baby is especially sleepy and nods off before finishing her meal consider breast compression to encourage her to continue nursing.
If everything else fails, your physician may consider the diagnosis of hypoplasia or insufficient glandular tissue. This is much more common in women with PCOS (polycystic ovarian syndrome). Check out this article about Insufficient Glandular Tissue.
What if the baby is getting enough milk, but still isn’t gaining weight?
Does your baby projectile vomit? Does he have green poops? Is she actually taking in enough breastmilk (confirmed by a lactation consultant or your physician), but still isn’t gaining weight?
It’s time to consider what’s in your milk. Green stools, projectile vomiting, blood or mucus in the stools, irritability around nursing, even reflux can be a sign that the baby isn’t tolerating your milk properly. The first thing I like to rule out is something called Milk Protein Allergy. This is a condition where the infant develops antibodies to cow’s milk proteins that are found in Mom’s breastmilk. It is by far the most common “intolerance” in breastfed babies, and is one of few evidence-based elimination diets for nursing Moms. To see if cow’s milk is bothering your baby you simply need to eliminate all cow’s milk products from your diet for a full two weeks. Please note that it does take 2 full weeks to see a difference. Make sure you eliminate all products including cheese, milk, whey, ice-cream, coffee drinks with milk (like latte’s and frappuccinos), cream, butter, and any packaged product that lists “casein.”
You can also experiment with other food eliminations like soy, gluten, tomatoes, citrus, corn, eggs, coffee and chocolate. I usually only recommend strict elimination diets as a last resort, however. Elimination diets in general (other than cow’s milk) have very minimal research supporting them, and often lead to a Mom needlessly restricting her diet. (And sometimes desperately needed calories!) I’ll try to do another blog post soon summarizing which foods actually have been shown to cause symptoms in recent research.
If you’ve ruled out all milk-related causes of failure to thrive then it is definitely time to bring in an expert – see the What to do if your child drops on their growth curve or is diagnosed with Failure To Thrive section under “What if my child is eating enough but still has failure to thrive?”
Finally: have a team of experts
I’ve mentioned this many times before! Have a team working with you! This may include your child’s primary care doctor, a lactation consultant, home-visit nurses and possibly other practitioners. (Like a speech language pathologist to improve sucking/swallowing. SLP’s are the “mouth” experts.)
References (in addition to the links above):
Meyer, Kathryn BA, RN; Anderson, Gene Cranston PhD, RN, FAAN. Using Kangaroo Care in a Clinical Setting with Fullterm Infants Having Breastfeeding Difficulties. MCN, American Journal of Maternal Child Nursing: July/August 1999 – Volume 24 – Issue 4 – pp 190-192
Kirkland R, Motil K. Failure to thrive (undernutrition) in children younger than two years: Management. UpToDate. 12 March 2014. Web. 30 August 2015.
Schanler, R J et al. Initiation of breastfeeding. UpToDate 9 September 2015. Web. 17 September 2015






Pingback: When Breastfeeding is NOT the Best Choice | Baby Chick
January 13, 2018 at 9:06 pm