
Don’t suppress that fever! (and why I don’t like Tylenol)
Annika, my 9 month old, got her first fever over Christmas. It went up to 105.8° F (on a temporal artery thermometer).
I can just hear the other parents now: “Yikes! 105.8? You gave her Tylenol, right?”
Nope. No Tylenol, no ibuprofen, nothing but extra cuddles and lots of nursing.
Her fever broke on its own a few hours later, and the next morning she was crawling around fast as her little knees could take her.
Fevers are not dangerous. The infection may be!
It’s not unusual for children to have very high fevers. In fact, it is generally very helpful for kids to get robust fevers, as it signals a strong immune response which can quickly eliminate pathogens (the bad bugs). A fever isn’t intrinsically dangerous until it reaches 108° F (yikes that is high!), as that is the point at which brain damage can occur.
Febrile (fever) seizures can occur at temperatures below this point. Despite the fact that they are unbelievably scary, febrile seizures alone are not a reason to give Tylenol or other fever-reducers. In fact, febrile seizures in otherwise normal children are completely safe. (Except that they may raise the parent’s blood pressure!)
Many parents mistakenly give their children fever-reducing agents thinking that it is the best thing for their child. In fact, many parents give Tylenol before their child has a fever! Remember that it is not considered a fever until the temperature reaches greater than 100.4° F with a rectal, ear or temporal thermometer, or greater than 100° F with an oral thermometer. (Rectal, ear and temporal thermometers are generally about a degree higher than oral thermometers. That’s why the 105.8 degree temporal reading didn’t worry me as much.) Anything under that reading is considered a normal variation in body temperature.
Here are some guidelines for managing a high fever:
1. Pay more attention to how the child is looking/feeling than what the thermometer says. A really sick looking kid is really sick, no matter what the temperature (high or low!). Sometimes kids will get listless, stop crying, and cannot be stimulated. Other times they will be incredibly irritable and cry uncontrollably. Use your best Mom (or Dad) radar and follow your instincts!
2. Normal fevers are between 100 and 104° F. Check with your child’s physician if it is higher than this. Often times it will be just like Annika’s story and we can wait it out, but once in a blue moon a dangerous situation can arise suddenly.
3. Wait on the Tylenol. The brain has a set-point at which fever tops out – it is totally a myth that without treatment a fever will keep rising indefinitely. Another myth: breaking the fever will stop the infection. In fact, the cytokines that cause fever also signal the immune system to do its job – we don’t want to interfere with that process!
4. AGAIN – how your child looks is the most important determinant of whether your child has a serious infection. Repeat after me: “It is not the number, but how my child looks that is important.”
5. All that said: it is NEVER normal for a newborn to have a fever. Any infant under age 3 months with a fever (greater than 100.4° F) needs to be checked out immediately.
Don’t believe me? Check out this great article from Seattle Children’s Hospital: Myths vs. Facts
Why I don’t like Tylenol.
Any why does Dr. Erika not like Tylenol? Oh this is a favorite subject of mine. I truly loathe acetaminophen as an OTC drug (no fault to the makers of Tylenol, they’re just doing their job). I have a whole long blog post (Just say “NO” to Tylenol: Acetaminophen causes autism?), but here is the simplified version:
Acetaminophen is hugely liver toxic. And I don’t mean in a vague, naturopathic “oh that McDonald’s hamburger is bad for your liver.” Acetaminophen is the number 1 cause of liver failure in the UK, and the number 2 cause in the US (of cases requiring liver transplantation). It is more common than viral hepatitis leading to acute (sudden) liver failure.
Why? The liver converts acetaminophen into N-acetyl-p-benzoquinone imine (NAPQI) in an attempt to get rid of it. (“N-acetyl what??” Don’t worry about pronouncing it, there will be no test at the end of this blog). The problem is that NAPQI requires huge amounts of a really important endogenous (body-made) antioxidant called glutathione in order to make it less toxic. Glutathione is responsible for scavenging all the free radicals produced all over the body by various (often normal!) metabolic processes. NAPQI chews up glutathione in massive quantities, leaving excess free radicals to burn and cause DNA and cellular damage all over the body. The liver then has to deal with not only the lack of glutathione, but the highly toxic NAPQI. Hepatocellular (liver cell) damage, necrosis (ugly cell death), and liver failure follows.
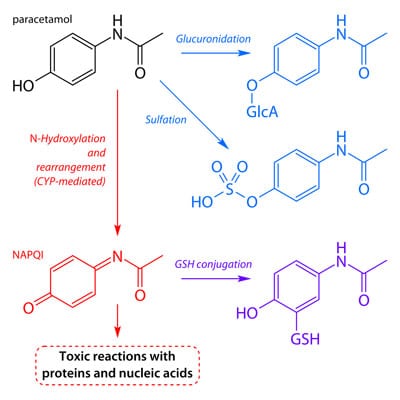
Okay, so you’ve taken Tylenol in the past and you didn’t die, so no harm, no foul, right? Sort of. The liver is an incredibly resilient organ, so in most normal people it takes the hit, waits until the acetaminophen passes, restores glutathione (if you eat right) and then rebuilds liver cells. BUT, in small children, in anyone with liver damage, or in large doses it can lead to liver failure.
Acetaminophen has a much lower maximum daily dose than almost any other over the counter medication. Adults should take NO MORE than 3,000 mg per day. That is six 500-mg pills per day. Children’s dose is at maximum 80 mg/kg per day. Most people have no idea what that means, which is why pediatricians give you a dosing chart. Do NOT exceed that dose!! The problem is that acetaminophen is in many combination products, including over the counter cough syrups, Nyquil, pain formulas and more. Read the labels carefully!
I have more reasons to loathe acetaminophen, including the implications of depleting glutathione in developing children. Here is that follow-up blog post again: Just say “NO” to Tylenol: Acetaminophen causes autism?
Until then, here’s your review:
1. It’s not the degree of fever, but how your child looks that matters.
2. Avoid acetaminophen whenever possible. When you do use it, read the label carefully and never exceed the recommended amount. Check all your pain, flu and fever combination products for their active ingredients, and never combine Tylenol with other over-the-counter formulas.
Don’t believe me? Here’s a great article from Seattle Children’s Hospital about the Myths of Fever: https://www.seattlechildrens.org/conditions/a-z/fever-myths-versus-facts/
And here is another great post, written by my colleague, about how to overcome your Fever Phobia.






Ryann Seay
November 14, 2022 at 7:27 amWhat are some alternatives to Tylenol when it comes to fevers?
Also, my 4yr old just had cataract surgery (hopefully his last) instead of using Tylenol/ibuprofen to manage the pain; what could I have used to help him?
I’m incredibly interested in learning more. I have been cutting sooo much out of my kids (and mine) foods and adding in better dye free options and alternatives.
Erika Krumbeck, ND
November 16, 2022 at 9:29 amHi Ryann,
I’m working on an e-book right now that explains how to use certain herbs instead of Tylenol or Ibuprofen. We have some of those included in our free e-book if you sign up for our newsletter. The longer e-book I’m working on will go into more detail!
~Dr. Erika
Martha
May 16, 2022 at 9:26 pmAny alternatives for reducing fever? My children suffer from febril seizures and I want to avoid those that’s why I always use Tylenol.
Jesslyn Kelly
April 4, 2021 at 4:33 pmThe link for the Seattle Children’s hospital is not working again, here is the updated one: https://www.seattlechildrens.org/conditions/a-z/fever-myths-versus-facts/
Erika Krumbeck, ND
April 7, 2021 at 10:39 amThank you!
Fabiana
September 1, 2020 at 8:38 pmThe link for the Seattle Children’s Hospital is broken. Can you provide the right one?
I would like to know if you can do a virtual appointment.
Tks/Fabiana
Erika Krumbeck, ND
September 8, 2020 at 9:38 amThanks Fabiana! I fixed it!
Cher
March 19, 2020 at 10:18 amCan you link me to some studies showing where Tylenol depletes glutathione? Thanks!
Erika Krumbeck, ND
April 1, 2020 at 2:04 pmTylenol (acetaminophen) directly uses glutathione (abbreviated GSH in many studies) in the process of detoxification in the liver. This considered common knowledge in the scientific community, so I’m not even sure if there are any studies “proving” it anymore. (Sort-of like proving the sky is blue?)
But here is the best article that describes what is happening: https://www.ncbi.nlm.nih.gov/pubmed/30471141
Pingback: 5 Lifechanging Ways to Use Essential Oils for Pregnancy – She Births Bravely
February 13, 2020 at 1:00 amPingback: What's In My Natural Wellness Cabinet | Mississippi Kitchen
November 2, 2019 at 6:39 am